That grumbling in your stomach, the eager anticipation for your next meal… what happens when it’s just not there? In our modern world of abundant food, a lack of appetite can be confusing. We’re told to “eat less,” but when your body genuinely doesn’t signal for food, it can be a cause for concern.
While Western medicine might look at stress, digestive disorders, or hormonal issues, Traditional Chinese Medicine (TCM) views a low appetite as a clear message from your body. It’s a sign that your digestive “fire” is low, your energy is lagging, and your system might be getting bogged down.
Let’s dive into the three core TCM reasons why your appetite has gone missing.
The Core Engine: Your Spleen Qi
In TCM, the Spleen is the star of the digestive show. It’s not the anatomical spleen of Western medicine, but a functional system responsible for transforming the food and drink you consume into usable energy (Qi) and blood. Think of your Spleen Qi as your metabolic furnace.
When your Spleen Qi is strong and abundant, this furnace burns brightly. It efficiently “cooks” your food, extracting essential nutrients, phytochemicals, and minerals to send around the body to power all your activities. A strong Spleen Qi means a healthy, regular appetite.
When your Spleen Qi is weak, the furnace is barely flickering. It doesn’t have the energy to transform food properly. The body, in its wisdom, recognizes this and says, “Don’t send more fuel, I can’t handle it!” The result? A lack of appetite, bloating after eating, fatigue, and loose stools.
So, the most fundamental reason for no appetite is simply this: your digestive engine doesn’t have the spark to get going.
The Symptom of a “Slow Metabolism”
You’ve likely heard the term “slow metabolism.” In TCM, this is a perfect description of Spleen Qi Deficiency. A slow metabolism isn’t just about burning calories slowly; it’s about the entire process of transformation and transportation being sluggish.
- Weak Spleen Qi = Slow Digestion = Slow Metabolism.
- This leads to poor nutrient absorption, low energy, and a tendency to feel heavy and lethargic.
That feeling of being “weighed down” after a meal, even a small one, is a classic sign that your Spleen is working overtime with limited resources. Your lack of appetite is your body’s natural brake pedal, trying to protect an already overburdened system.
The Dampness Connection: When the System Gets “Bogged Down”
This is where it gets really interesting. A weak Spleen doesn’t just lead to low energy; it also causes problems with water metabolism.
A healthy Spleen helps to move and transform fluids in the body. When the Spleen is weak, these fluids aren’t processed properly and begin to accumulate as Dampness. Imagine a swamp forming in your digestive tract.
Dampness is heavy, sticky, and obstructive. It smothers the digestive fire, making the problem even worse.
How does this feel?
- A feeling of fullness in your stomach, even if you haven’t eaten much.
- A complete absence of hunger or even a slight nausea.
- A heavy feeling in your limbs and brain fog.
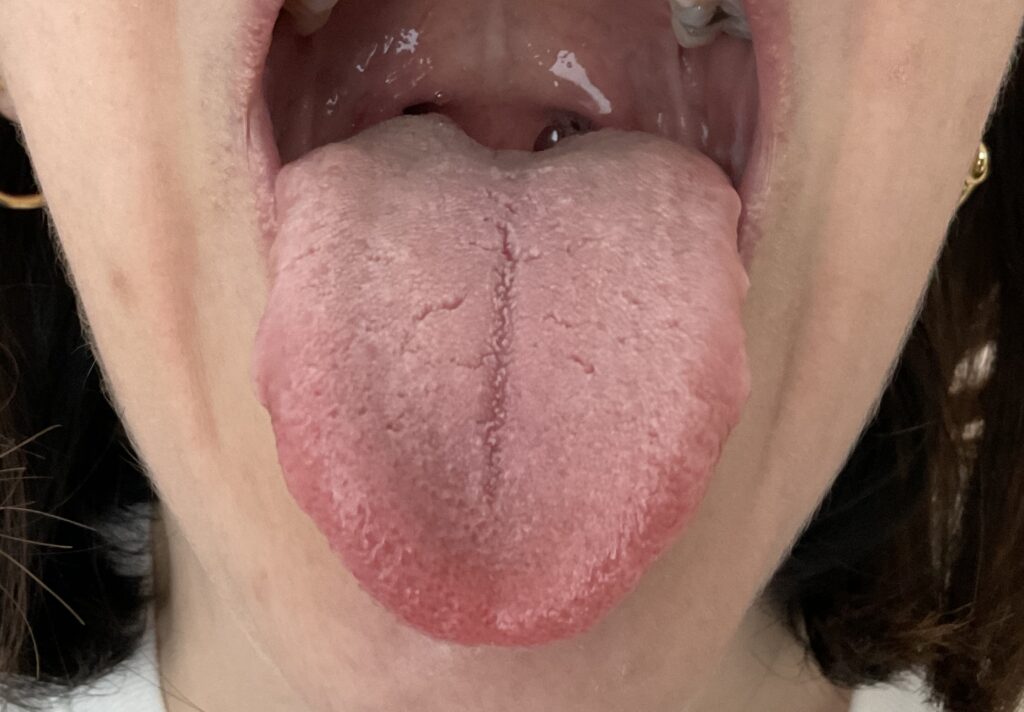
- A thick, greasy coating on your tongue.
When Dampness is present, your body isn’t just saying, “I’m not hungry.” It’s saying, “I’m already bogged down and stagnant. Don’t add to the problem.“ The lack of appetite is a direct result of this internal “swamp” quenching your digestive fire.
This also explains a common frustration: why someone can be carrying excess weight yet have no appetite and still struggle to lose it. In TCM, this isn’t necessarily about consuming too many calories, but about a metabolic system that is so bogged down by Dampness that it cannot properly process any food or burn stored energy efficiently. The body, in its stagnant state, holds onto this damp, heavy energy (the excess weight) because the Spleen simply doesn’t have the strength to transform and move it.”
What You Can Do to Stoke Your Digestive Fire
The good news is that you can support your Spleen Qi, dry up Dampness, and rekindle your appetite with simple dietary and lifestyle shifts.
- Choose Warm, Cooked Foods: Your weak Spleen furnace struggles with cold, raw foods. Think soups, stews, steamed vegetables, and warm porridge. These are pre-digested, easy-to-transform meals.
- Incorporate Qi-Strengthening Foods: Gently incorporate foods like sweet potatoes, squash, carrots, brown rice, oats, and well-cooked legumes.
- Limit Damp-Forming Foods: The biggest culprits are dairy, sugar, refined carbs, fried foods, and highly processed items. These directly weaken the Spleen and create Dampness.
- Eat Mindfully and Regularly: Don’t skip meals. Eat at consistent times to train your body. Sit down, chew thoroughly, and avoid working or watching TV while you eat. This directs energy to your digestion.
- Move Gently: Light exercise like walking or Qi Gong helps to move Qi and resolve stagnation, supporting your Spleen’s function.
Listening to your body is a form of wisdom. A lack of appetite isn’t something to ignore or force through. In the language of TCM, it’s a clear signal that your core metabolic engine needs support. By understanding the connection between Spleen Qi, a slow metabolism, and Dampness, you can take gentle, effective steps to rekindle your inner fire and welcome back a healthy, natural hunger.
As always, this information is for educational purposes. If you are experiencing a persistent lack of appetite, please consult with a healthcare professional or book a consultation at Aetherium Acupuncture & Integrative Medicine for a personalized diagnosis and treatment plan.